Tuberous breasts
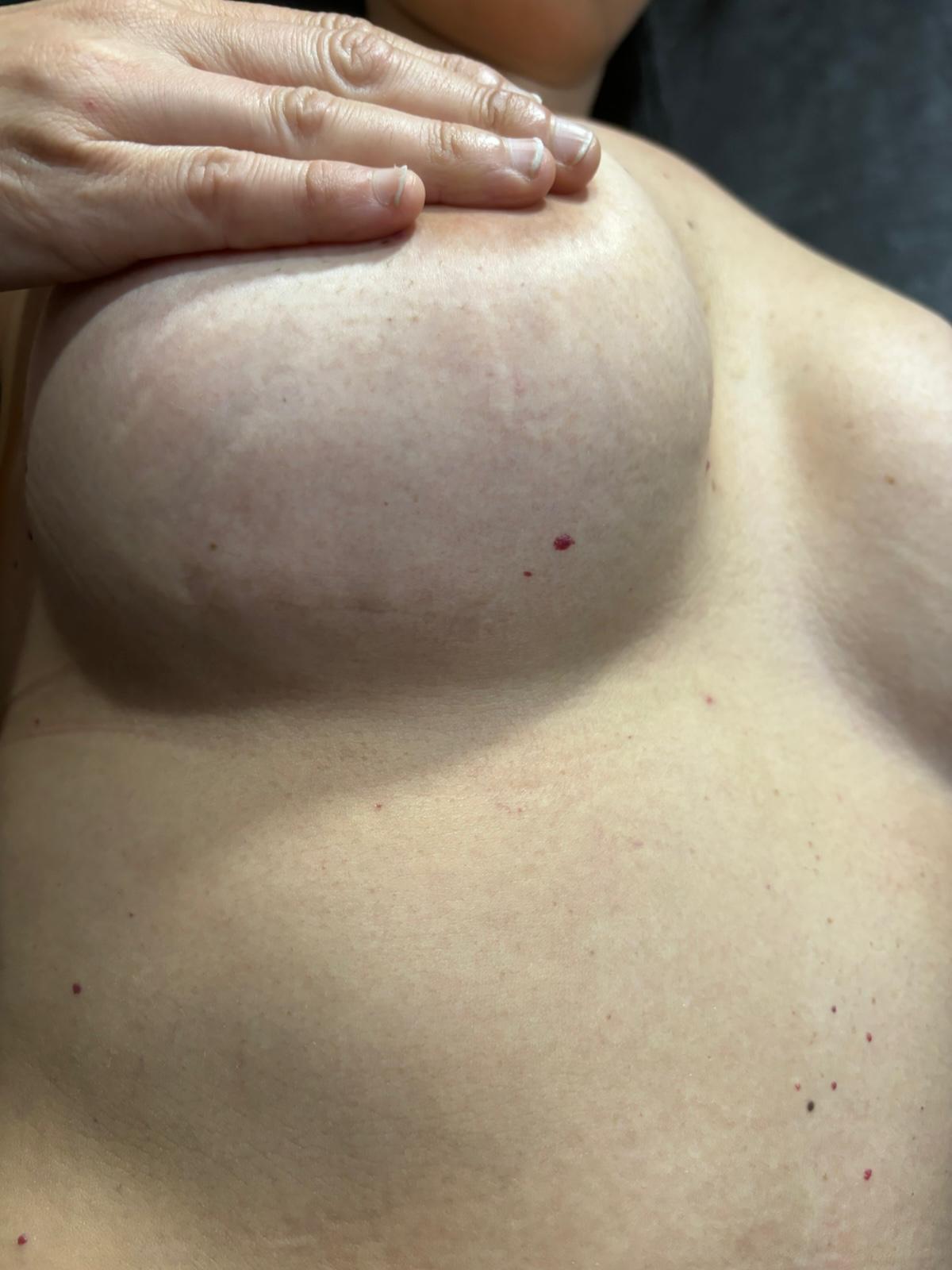
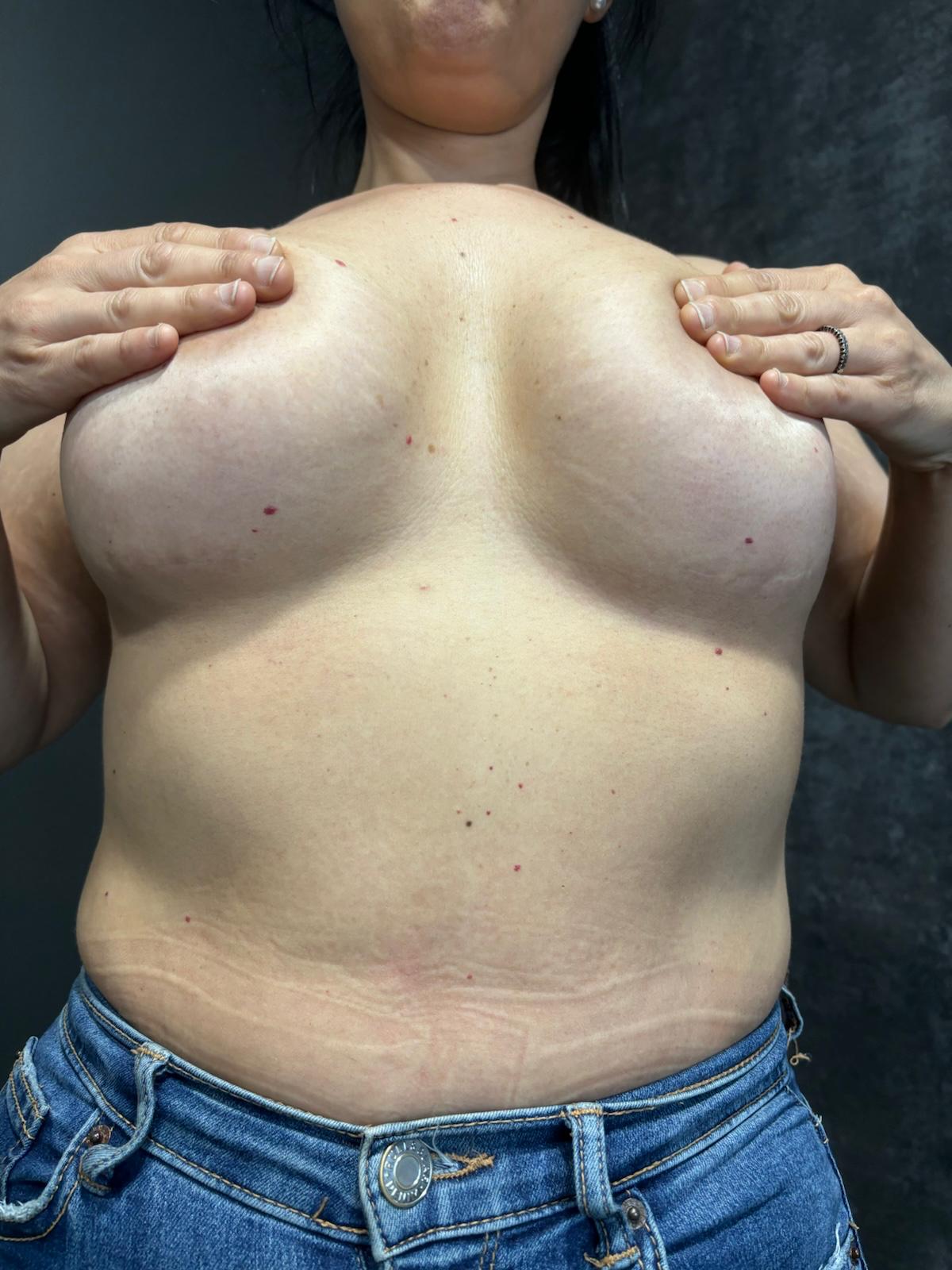
Tuberous breasts, also known as tubular or tube-shaped breasts, are a rare anatomical variation in breast shape characterized by a narrow base and poor development of the lower part of the breast, resulting in a conical or elongated appearance. It is a congenital deformity that affects the aesthetics of the breast, a condition that can cause physical discomfort and affect the self-esteem of women who experience it.
There are different degrees of tuberous breasts, but their main characteristics compared to normal breasts are:
✔️ Clear asymmetry between one breast and the other
✔️ Wide areolas due to herniation of breast tissue
✔️ Constricted breast implant base, especially in the lower poles of the breast

Correction of tuberous breasts is possible through a combination of surgical techniques including redistribution of breast tissue, correction of narrow base, and in some cases, placement of breast implants. During the initial consultation, the patient’s unique anatomy will be evaluated and aesthetic goals will be outlined to determine the most appropriate approach.
In some cases of tuberous breasts, it is possible to achieve satisfactory results without the use of breast implants thanks to the redistribution of breast tissue and correction of the narrow base that help improve the shape and projection of the breasts, creating a more natural and balanced appearance.
However, using prostheses is usually the most common practice and injections of the patient’s own fat are also often used, combined or not with breast prostheses. Prostheses can help increase volume and create a more rounded and proportional appearance, correcting the lack of development in the lower part of the breast and improving the symmetry between both breasts.
In the operating room we use the most advanced tissue remodeling techniques to achieve optimal and satisfactory results in a completely safe and effective manner.
B/A Case 1
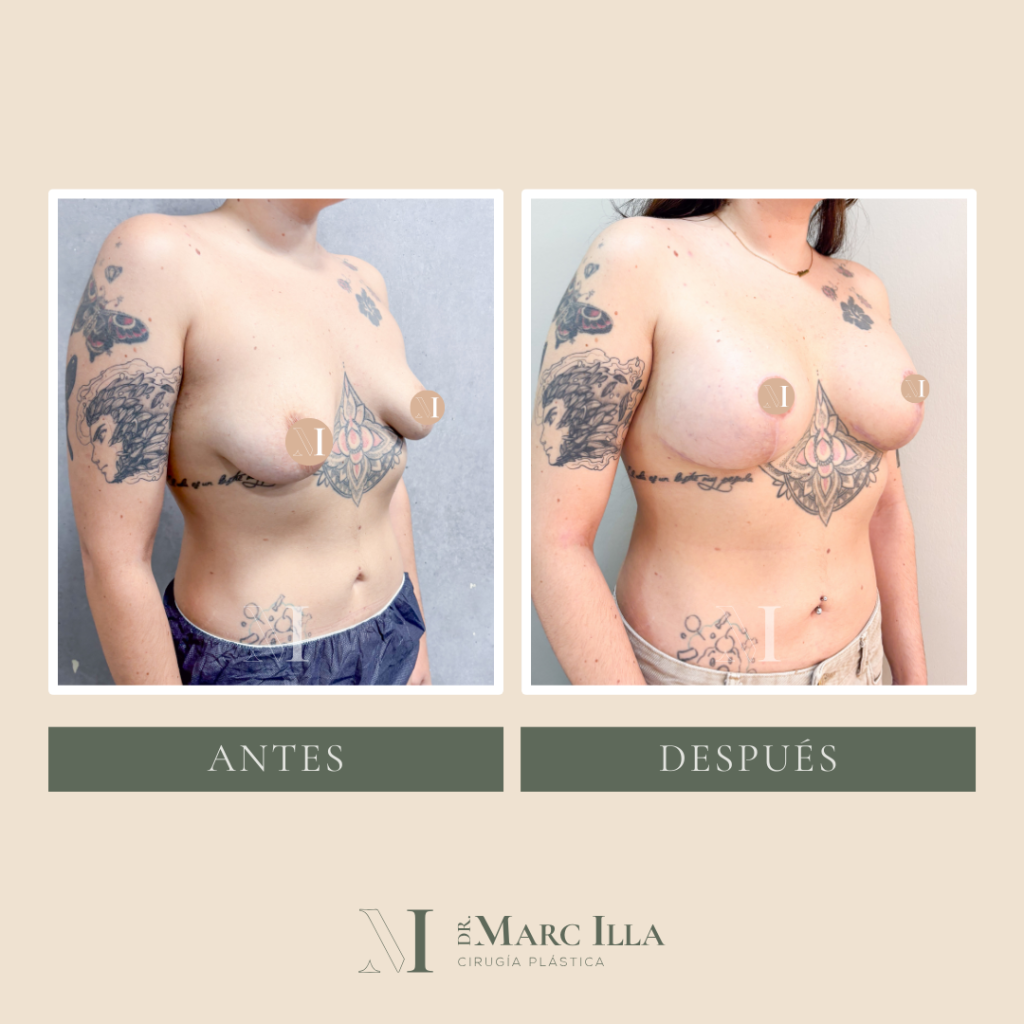
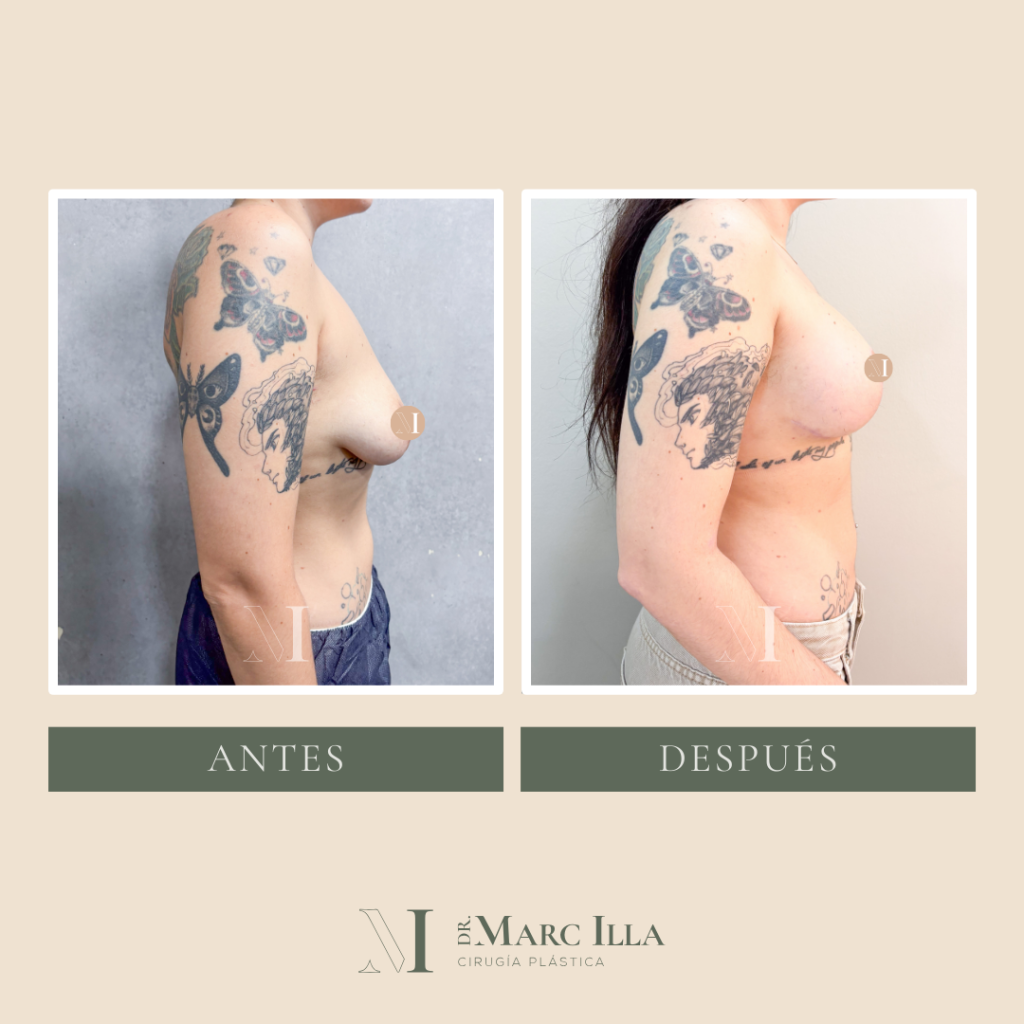
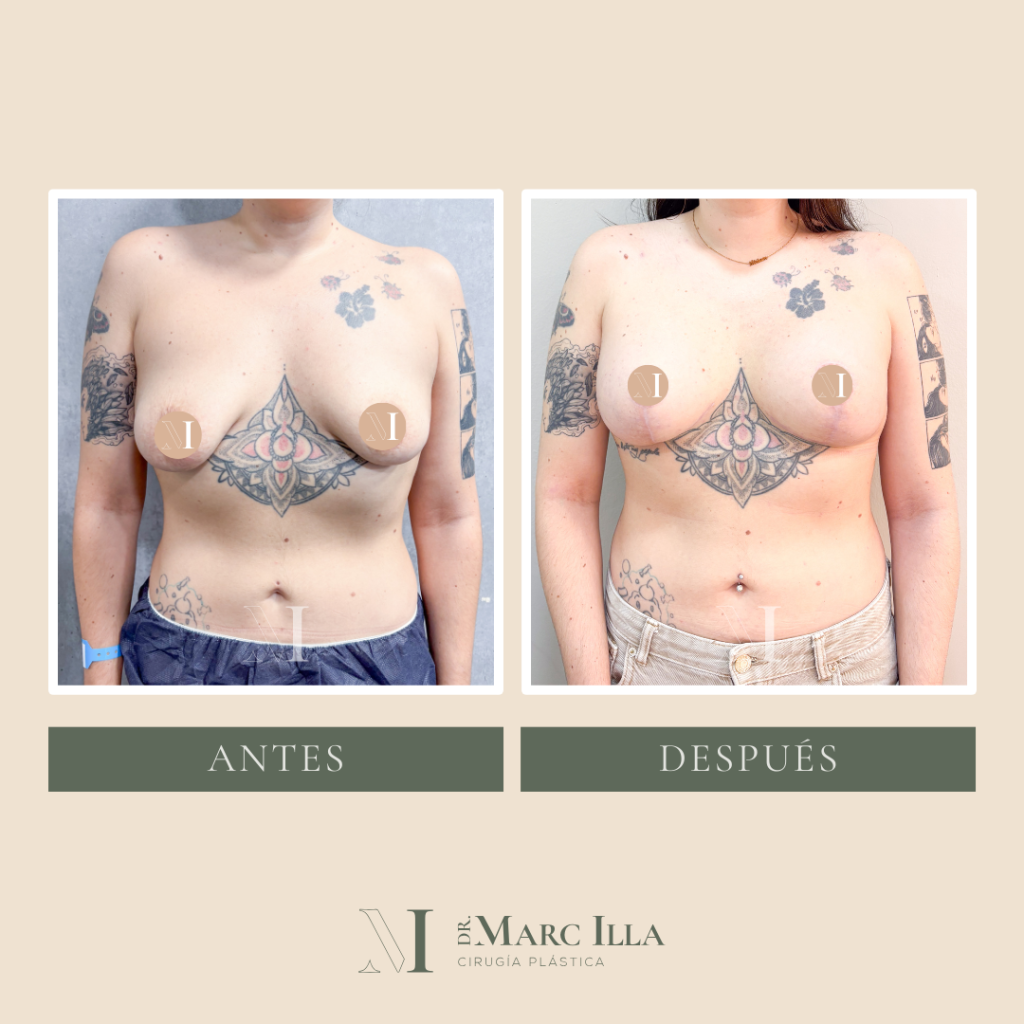
B/A Case 2



B/A Case 3



How are tuberous breasts corrected?
Correction of tuberous breasts generally involves a combination of surgical techniques to address the specific characteristics of this breast malformation.
¿Qué es exactamente una mama tuberosa?
¿Cuáles son las causas de las mamas tuberosas?
¿Cómo se diagnostican las mamas tuberosas?
¿Qué opciones de tratamiento existen para las mamas tuberosas?
Do you think you have tuberous breasts?
Classification of tuberous breast deformity
The von Heimburg classification of tuberous breasts is one of the methodologies used to categorize this type of breast malformation. Von Heimburg proposed a classification that considers several anatomical aspects and characteristics of the tuberous breast. This classification is based on three main types of tuberous breasts:
Frequently Asked Questions
The prognosis after treatment for tuberous breasts is usually favorable. Corrective surgery can significantly improve the shape and appearance of the breasts, which can have a positive impact on the patient's self-esteem and quality of life.
There are several tricks that can help us achieve an aesthetically pleasing neckline.
- Choosing the prosthesis: This is the most important thing to be able to create a good cleavage. It is necessary that the width is sufficient to cover the entire thorax and thus be able to correctly occupy the entire area. The shape, level of implantation and size of the patient's previous breast must also be taken into account.
- The way in which the pectoral muscle is lifted: this is where the prosthesis is inserted and the muscle itself can help us bring the breasts together.
- Internal Bra: With the help of stitches, we fix and close the edges of the prosthesis pocket well to create an internal bra effect.
- Lipoinjection: Fat injection into the breast allows for the creation of a completely natural volume and avoids long-term aesthetic defects such as rippling (irregularities in the surface). It allows us to create a beautiful and natural neckline with the patient's own fat.
The answer is: IT DEPENDS on each case
When to decide “NOT to wait to be a mother”? This is the preferred option for patients who do not feel comfortable or identified with the shape and/or volume of their breasts at the moment. For many patients, for example at 20 years of age, it is not worth spending another 10-15 years (until the age at which they want to be mothers) with a breast that does not feel good. It is true that the breast changes over the years, with sudden weight changes or pregnancies, but retouching a breast that has already been operated on tends to be simpler. These are usually surgeries that mainly affect the skin and fat without having to touch deep areas or previous breast prostheses. Hospital admission is not usually necessary and the postoperative period is usually very bearable. For this reason, many patients decide not to wait and to operate on their breasts at the moment when they do not feel comfortable with them.
This option is best for women who only want to undergo surgery once. In this case, it is best to wait until you have had all the children you want before undergoing breast surgery. The price to pay will be spending several more years accepting the shape and volume of the breasts that you are not completely comfortable with.
It is possible that it may have an effect, but it cannot be guaranteed. The intervention involves the removal of breast tissue and the replacement of the nipple. It will depend on the type of surgery (whether more or less breast tissue is preserved under the nipple structure) and the patient's genetics (there are patients who have little mammary gland but produce a lot of breast milk, this usually depends more on how much the mother is stimulated and not so much on genetics or the amount of mammary gland left in the surgery).
However, the amount may be smaller or there may be additional difficulties due to changes in the structure of the mammary gland.
This type of surgery involves remodelling the mammary gland and, usually, also the skin of the breasts. For this reason, it is common to have alterations in sensitivity that usually last at least for the first 6 months, then they usually recover within 12-18 months.
Patients would like to know the exact result of their surgery. While it is true that the results of surgery (and of any medical intervention) have a predictable part (it will depend on the type of intervention planned, the wishes of the patient, and factors that we study in the physical examination such as the quality of the tissues), there is another unpredictable part that can modify the result, such as the underlying genetics of each patient or other factors that we have not been able to identify initially.
Our goal is to minimize these unforeseen factors that may affect the result we leave in the operating room in order to give the patient an idea as close as possible to what they will achieve, but it is impossible to guarantee a 100% result for this reason.
- Minors under 18 years of age with aesthetic objectives (in tuberous breasts, surgery can be performed before the age of 18, always with parental consent)
- Pregnancy
- Active or past breast infection within the last 6 months.
- Any uncontrolled disease
Breast mammograms can be performed without problems in women who have breast implants. We recommend that they be performed 12 months after the operation to prevent inflammation from the surgery from interfering with the interpretation of the test. As long as you notify the doctor who is requesting the test in advance so that it can be scheduled to be performed using the Eklund technique, a maneuver that consists of moving the prosthesis towards the back of the breast, leaving it outside the compression paddle, compressing only the breast tissue to perform the mammogram. There is no problem with doing other tests such as MRIs or flying (the prostheses do not explode). Being a breast implant wearer is even beneficial for breast self-palpation, since the breast tissue is more taut and distributed around the implant and allows for greater sensitivity and specificity when palpating all this tissue.
No, the quality of the materials used to manufacture the breast prostheses we work with has allowed us to reduce the risk of complications associated with these to a very low level. This does not mean that it may not be necessary to replace the prosthesis or remove it during life for some reason, but this is rare. The prostheses used years ago did recommend changing them every 10 years, but thanks to scientific advances this is no longer the case.
No type of plastic surgery is related to an increased risk of cancer. The use of breast implants has been linked to some types of autoimmune disease or some types of lymphoma, but there is no scientifically clear or proven relationship with the breast implants we currently use (it has happened with some brands of breast implants used in the past).
General anesthesia is always used to ensure patient comfort and to allow the surgeon to work with maximum precision and safety. Full intubation is not usually necessary; a laryngeal mask with mild anesthesia is usually the route of choice for our anesthesiology team. Breast surgery should not be performed with local anesthesia; it is bad practice. Throughout the entire operation, the patient's general condition and vital signs are monitored and taken care of in the utmost detail by our anesthesiology team.
An overnight stay is usual. It is preferred to be under health surveillance for the first few hours. Although it is not a long or risky surgery, we have gone through an operating room and received medication. In addition, intravenous medication is useful in the first hours to maximize the patient's postoperative comfort.
We work with different brands of breast prostheses: Motiva, Silimed, Politech, Eurosilicon, Nagor… None of them are the same as the other, each brand has its pros and cons that must be assessed. We will specifically study your case to choose the breast prosthesis that is best for achieving the result you are looking for.
The answer to this question must be individualized in each case. Even so, it can be said that in most patients the recommendation is to place the prosthesis under the muscle (also called submuscular or subpectoral, since the muscle used is the pectoralis major). Among the most common ways of placing a prosthesis under the muscle, the most commonly used is the dual plane, where 50-75% of the prosthesis is covered by the muscle and 25-50% by the lower part of the mammary gland.
This placement has several advantages: the anatomical structure of the mammary gland is not touched at all, which means that sensitivity and subsequent ability to breastfeed are better preserved, and it is a cleaner surgery, which reduces the risk of infection or capsular contracture.
Placing the prosthesis above the muscle, although not very common in our normal practice, in certain patients, has certain advantages that must be assessed in each case. Above the muscle, it can be done in two ways: subglandular (directly under the mammary gland) or subfascial (under the first layer that surrounds the pectoralis major muscle).
This is a very common question in consultations, since, as is normal, patients would like to know the exact result of their surgery. While it is true that the results of surgeries (and of any medical intervention) have a predictable part (it will depend on the type of intervention planned, the wishes of the patient, and factors that we study in the physical examination such as the quality of the tissues), there is another unpredictable part that can modify the result, such as the underlying genetics of each patient or other factors that we have not been able to identify initially. Our goal is to minimize these unpredictable factors that may affect the result we leave in the operating room in order to give the patient an idea as close as possible to what they will achieve, but it is impossible to guarantee a 100% result for this reason.
So… in answer to the question: What size bra will fit me? We won’t know the exact size until the swelling has gone down and we have a more or less stable result 3-6 months after surgery.
Did you know that 7 out of 10 women do not know their correct bra size?
30% of consultations about breast pain are due to wearing an inappropriate bra. Wearing the wrong bra size can cause not only discomfort, but also marks and injuries, as well as accelerating the ageing process of the breast.
Types of prostheses
There are different types of breast implants available, each with its own unique features and benefits.
The choice of one or another prosthesis It certainly depends on the individual aesthetic goals of each patient, as well as their anatomy and personal preferences. In consultation we work closely with each patient and We carry out a complete study of the shape and consistency of the breast and the shape and size of the thorax to determine the most suitable type of prosthesis to achieve the desired results and satisfy aesthetic needs.

Where can breast implants be placed?
Under the muscle (also called submuscular or subpectoral implant)): This is the majority of our cases. Among the most common ways of placing a prosthesis under the muscle, the most commonly used is the dual plane, where 50-75% of the prosthesis is covered by the muscle and 25-50% by the lower part of the mammary gland.
Above the muscle or subglandular implant (directly under the mammary gland) or subfascial (under the first layer surrounding the pectoralis major muscle). This technique is less common, but in certain patients it has certain advantages that must be assessed in each case.
Yes, indeed there is a scar.
This is what a scar in the crease of the breast (submammary fold) after breast augmentation with prostheses looks like at 2 years of age.
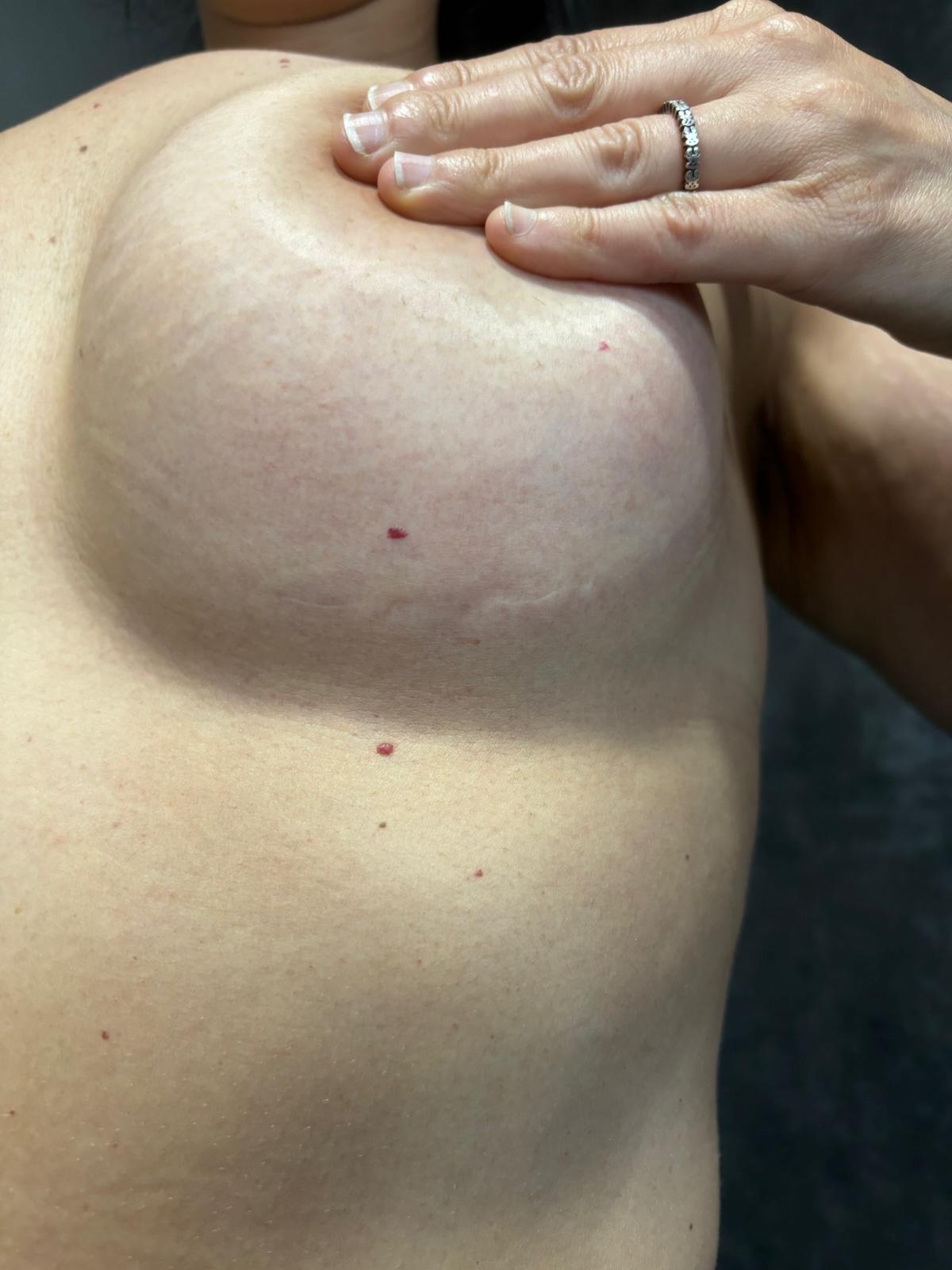
Postoperative
It is normal to experience pain, swelling, and tenderness in the breasts after surgery. Your plastic surgeon may prescribe pain medication to help manage discomfort for the first few days.
You will notice a pain that is usually described as “soreness”, as if you had gone to the gym three or four days in a row. The pain is usually very well tolerated, especially if you follow the medication regimen that we recommend taking the first week after surgery to the letter. Most patients explain that the discomfort is greater during the first 3 or 5 days, and then it is minimal; although each person has a different pain threshold.
After surgery, a compression bandage may be placed around the breasts to help reduce swelling and keep the breast implants in place. However, if the procedure was minor, the postoperative bra may be put on without a bandage to reduce discomfort for the patient.
The first postoperative hours are spent in the hospital's recovery area, where all vital signs are closely monitored. When the patient has fully woken up from the anesthesia (no longer groggy), the pain and dizziness are under control, and she is therefore in optimal condition, she is taken to her room with her family and friends. There, recovery begins in preparation for returning home. In her room on the ward, the nursing staff will diligently ensure that the patient is comfortable and with minimal discomfort, using the medication prescribed by our anesthesiology team when necessary. The nursing team will help the patient to tolerate the intake of liquids and solids, and walking, and thus ensure a safe return home. The next day we will come to the hospital to visit you, to check that the patient is in good general condition and that there are no complications of any kind in the areas that were operated on. We will consider the possibility of removing the drains and bandages, and if everything is in good condition, we will proceed to deliver the discharge report where we will detail all the postoperative instructions that the patient must follow and the prescriptions that she will need to give to the pharmacy in order to receive the medication that we recommend. In the first week after surgery, pain and dizziness are rare, but there are specific times when they can appear and you have to be prepared.
During the first three months (more pronounced during the first month) the breasts will appear higher and larger due to postoperative edema or swelling. It may even be that one breast is more swollen than the other and therefore appears larger (there are patients who have this swelling greater in one breast than in the other and it varies depending on the week and from one breast to the other) giving a sensation of asymmetry or deformity. After three months we have fairly stable results. The result of cosmetic surgery should not be considered definitive until a year has passed since the day of the intervention.
We have to consider them our allies, since they remove the liquid that causes a lot of inflammation if it stays inside and can even increase the risk of complications. They are a nuisance, but there is nothing worse than that. In many of our interventions we leave them, at least until discharge from the hospital. We always leave them longer in abdominal and back surgery than in breast surgery.
You can move your arms to do activities that do not require effort. The important thing is not to lift them or lift heavy weights. Normally we allow you to lift your arms from the second postoperative week, until the surgery is well healed on the inside and movement cannot affect it. And finally, you can lift heavy weights from the fourth postoperative week.
It depends on the type of job. Normally, we allow you to start computer work (secretarial work, IT, telecommunications, etc.) two weeks after surgery. Jobs that involve driving or a lot of movement usually start after three weeks.
We usually allow driving from three weeks postoperatively.
We recommend spending the first five to seven days postoperatively at home, after which we allow going out for a coffee or visiting family or friends. Driving or taking long walks from three weeks postoperatively. Sports such as going to the gym or running from four weeks postoperatively. Intense sports such as climbing, swimming, triathlon… from six weeks postoperatively.
Most stitches are subcutaneous or intradermal, that is, they are under the skin, they go inside. We do not normally leave external stitches (only those at the ends of the intradermal suture). If there is a need to leave an external stitch, we normally remove it after 7-15 days.
Unless there are any conditions that require a longer period of wear, we usually recommend wearing the sports bra for a month, both day and night.


